Merit Based Incentive Payment System
(MIPS)
By partnering with TriumpHealth for MIPS services, healthcare organizations can improve their overall quality of care and potentially earn incentives from Medicare.
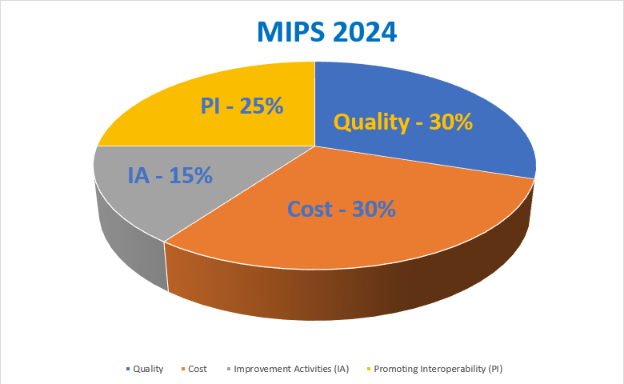
-

-

-

-

-

-

-

-

-

-

-

-

-

-

-

-

-

-

-

-

-







