Medical Billing & Revenue Cycle Management
What is Revenue Cycle Management?
Revenue Cycle Management (RCM) is the end-to-end process of managing a healthcare practice’s financial flow-from patient registration and appointment scheduling to claims submission, payment collection, and financial reporting.
With ever-changing regulations and complex payer requirements, partnering with an experienced RCM provider like TriumpHealth helps your practice prevent delays, minimize denials, and maximize revenue.
TriumpHealth’s Comprehensive Revenue Cycle Management Services
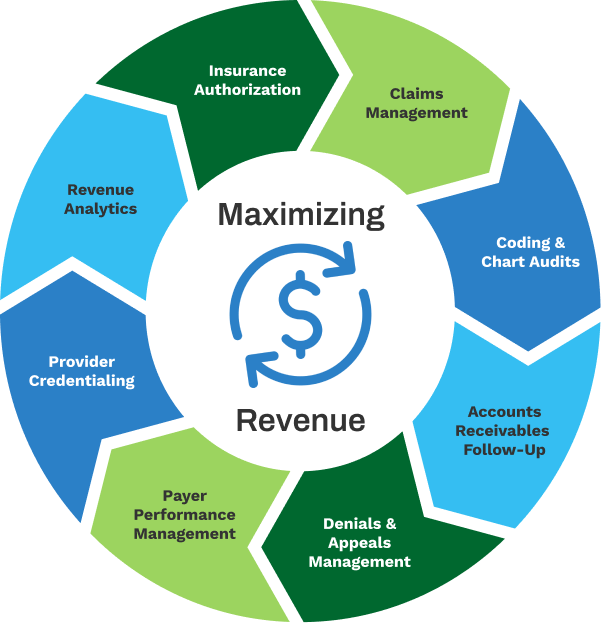
TriumpHealth offers complete medical billing and revenue cycle management solutions for every stage of the revenue cycle—from pre-authorization and claims submission to payment posting and financial reporting. We’ll take care of your cash flow, while you take care of your patients.

Charge Entry & Claims Management
Make every claim count with accurate charge entry. We ensure precise charge capture and timely, accurate claim submission so you’ll receive maximum reimbursement.
- Verify and enter charges accurately.
- Submit clean claims to reduce rejections.
- Monitor claims for timely adjudication.
What Makes TriumpHealth Revenue Cycle Management Services Different?
TriumpHealth helps healthcare providers reduce costs, improve efficiency, and maximize reimbursement through innovative medical billing and revenue cycle management solutions. Here’s what sets us apart:

Advanced Technology
Leverage cutting-edge tools for efficient and accurate medical billing.

Industry Expertise
Benefit from our team’s in-depth knowledge of payer rules and guidelines

Personalized Solutions
Tailored approaches to meet the unique needs of your medical practice.

Seamless Workflows
Experience smooth and efficient processes for optimal results.

Superior Results
Achieve excellence in medical billing with our proven track record of success.

Revenue Cycle Assessment
Optimal revenue cycle performance hinges on monitoring key performance indicators (KPIs).
Get Started with TriumpHealth Today
Contact us today to learn more about our comprehensive Revenue Cycle Management services and how we can support you.
By clicking ‘Submit,’ you agree to TriumpHealth’s Terms Of Service and TriumpHealth’s use of the information you have provided in accordance with our Privacy Policy.
Additionally, you agree to receive promotional phone calls or text messages from TriumpHealth at the phone number provided. Message and data rates may apply. You can STOP messaging by sending STOP and get more help by sending HELP.
Maximize Your Revenue. With Expert RCM Services
Schedule a consultation today to achieve financial success and regulatory compliance. Let us help you improve patient outcomes while increasing your revenue.










